By Motion Physical Therapist: Dr. Alyssa George, PT, DPT, OCS
Pregnancy and cesarean section can have a significant impact on your posture and muscle strength and may lead to urinary incontinence, pelvic girdle or back pain, and/or pelvic organ prolapse. Caring for a newborn typically requires static postures, lifting, carrying, and bending that require a significant amount of strength and stability throughout your pelvis, back, abdomen, neck, and shoulders. It is important to know how to safely re-train certain muscles post-cesarean so that you can perform these activities without pain. Physical therapy can significantly improve your ability to return to functional activities postpartum.
Rest is important to allow healing to occur following cesarean section. Normal, non-strenuous movements will not harm your stitches and it is important to listen to your body to determine which activities are safe.
Getting into and out of bed
When you turn over in bed, bend one knee at a time and support your belly with your hand or a small pillow if necessary while turning your shoulders, hips, and knees all at the same time to avoid excessive twisting. When getting into bed, keep shoulders, hips and knees facing the same direction while lowering your body down onto your side and bringing both feet up onto the bed together before rolling onto your back. Reverse this sequence when getting out of bed by rolling onto your side, lowering both legs off the side of the bed, and pushing up to a seated position with your arm.
Sitting and feeding
Whether you are breastfeeding or bottle feeding, make sure you have adequate support for your low back and use a cushion or pillow to bring your baby close to you to avoid slouching or leaning. Remember you can also lie on your side for feeding.
Coughing and sneezing
It is important to keep your chest clear. You can do this by taking a deep breath 2-3 times per hour. Your tummy may be sore but try not to hold back a cough or sneeze. To make these more comfortable, you can lean forward, resting your hands on your legs or bring your knees to your chest if you are lying in bed. Support your belly with your hands or a small pillow.
Posture
Try to stand tall and avoid slouching or leaning forward. When changing diapers, place your baby on a changing table that is high enough to avoid bending.
Exercises
It is important to not expect too much too soon. Your body needs time to heal. Avoid any activities that make you feel like you are straining. Do not lift anything heavier than your baby for the first few weeks. Walking is a great way to stay active. You can also start performing gentle pelvic floor muscle contractions when you feel ready. Regular use of these muscles can help improve normal bowel and bladder control, improve and prevent prolapse, and restore sexual function. Try contracting these muscles by tightening the muscles around your vagina as if you are trying to stop the flow of urine or gas while breathing out. Try holding this contraction for five seconds and repeating a few times per day. Use the same muscles to perform ten quick squeezes. Also try to contract these muscles before coughing, sneezing, and lifting. If you are unsure if you are performing these exercises correctly or if you have ongoing incontinence, it is a good idea to visit a pelvic floor physical therapist for guidance.
Six weeks after a cesarean section is typically when it is safe to return to gentle exercise but this will vary by person and it is best to check with your healthcare provider at your six-week postpartum follow-up visit. Once you have received the go-ahead, you can start to return to exercise but make sure you start slow and build gradually.
Scar management
Once your scar has healed completely, it can be beneficial to start doing some work to desensitize and stretch your scar.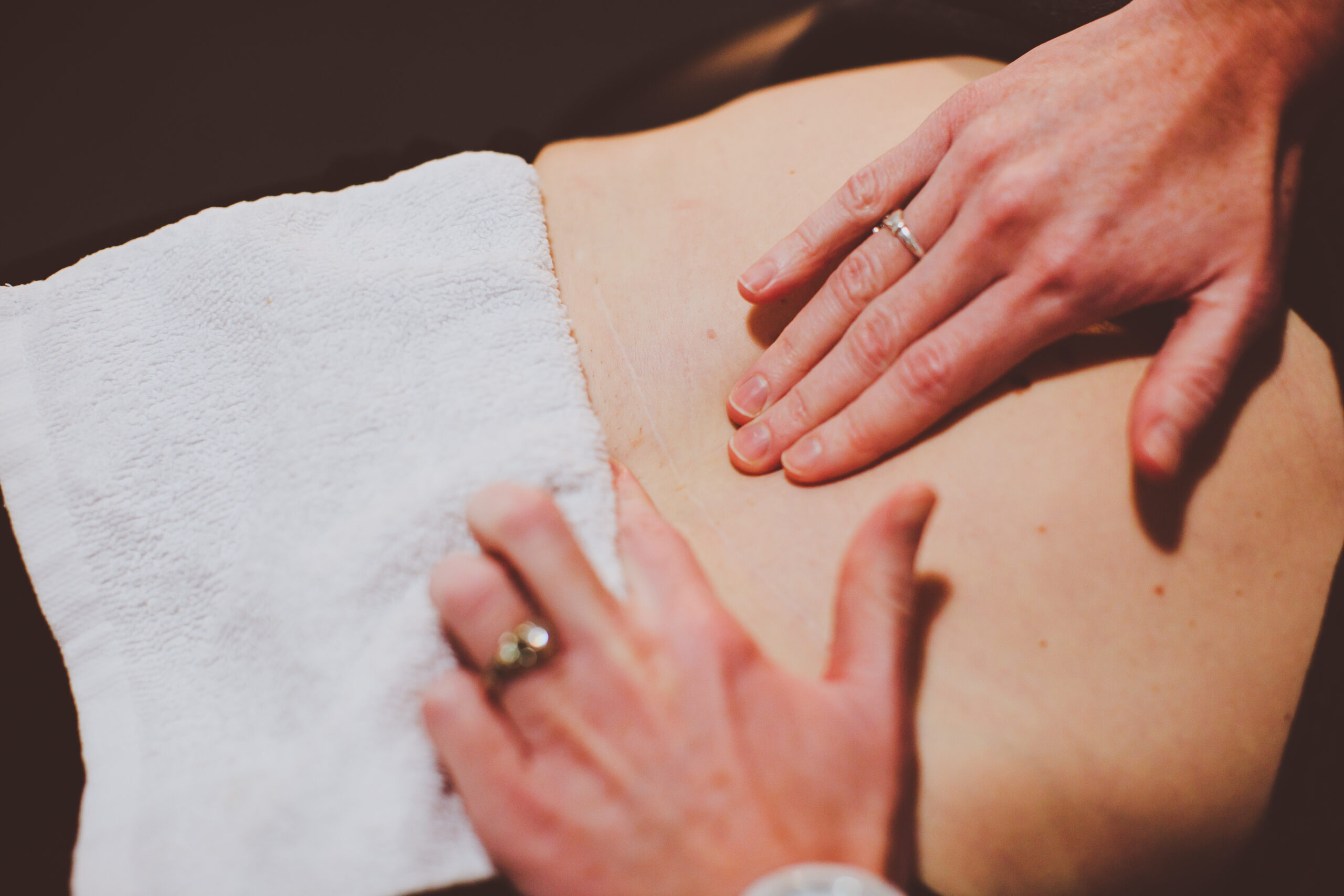
Abdominal scar tissue desensitization:
- Gently touch, tap, or pat the area with a progression of materials from soft to rough: (cotton ball, silky material, terry cloth, paper towel, soft velcro, soft loofah).
- Once gentle touch to the area with an item no longer elicits pain or sensitivity, begin to add sweeping or massaging motions (this progression will occur over time).
- Perform for 5-10 minutes several times per day.
Scar tissue stretching (can be started 6 weeks after surgery, only after the incision is fully healed):
- Anchor one side of scar with a finger
- Stretch scar by pulling in the opposite direction with another finger until resistance is felt.
- Hold 30-60 seconds. Repeat 2-5 times
- Switch anchor side and direction of stretch.
- If the scar itself is too sensitive, you can start an inch away from the scar and work up to it (Herrera 2010).
Dr. Alyssa George, PT, DPT, OCS

Alyssa wants to get you back to doing what you love, whether that be sports/recreational activities, your career, or caring for your family. Specializing in treating pelvic and orthopedic conditions, Alyssa develops individualized treatment plans because she understands that no two bodies are alike. She has been involved in research projects to help advance the field of physical therapy. Most recently she has written a case series detailing the benefits of dry needling for chronic pelvic pain and presented on the function of breathing muscles in pelvic pain at the American Physical Therapy Association’s Combined Sections Meeting. She has over nine years of experience as a physical therapist and has started and led pelvic health programs at clinics in Texas, Ohio, and now Minnesota, her home state.
Alyssa earned a Bachelor of Arts degree in biology from Gustavus Adolphus College, a Master of Physical Therapy degree from the University of Wisconsin-Madison, and continued her education at the University of Montana, earning her Doctorate in Physical Therapy. She is a board-certified clinical specialist in orthopedics and earned her certification in pelvic physical therapy from the American Physical Therapy Association Section on Women’s Health. She has been a lecturer and faculty mentor of both orthopedic residency and manual therapy fellowship programs at The Ohio State University and is a credentialed clinical instructor for physical therapy students. Alyssa has been certified in dry needling and utilizes other various manual therapy techniques in her management of abdominopelvic disorders (including incontinence, constipation, lumbopelvic pain, and pregnancy-related musculoskeletal disorders) and orthopedic conditions of the neck, back, shoulder, hip, knee, and foot/ankle.
Schedule an Appointment with Dr. Alyssa Today for a More In-Depth Assessment
References
Herrera I. Ending Female Pain. Duplex Publishing 2010.